WHAT IS MRKH?
‘Only when we are no longer afraid, do we begin to live’
MRKH (Mayer-Rokitansky-Küster-Hauser) Syndrome is a congenital condition (present at birth) that affects around 1 in 5000 female births.
Whilst everyone is different, we have provided a summary of how MRKH usually affects the body and how it is typically diagnosed.
Please note, the information on this page is for background information, and not a replacement for qualified advice about your individual case.
You may wish to also visit our Life without Children, Path to Parenthood pages
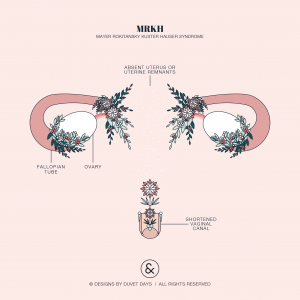
MRKH is a disorder of reproductive development leading to the absence of the uterus, cervix, and the shortening of the vagina.
The presence of ovaries produce female hormones that lead to breasts and pubic hair developing. However, the absence of the uterus means that periods don’t start, which is usually the first sign investigated by a local doctor or physician. Most will then usually be referred to see a specialist in gynaecology, where they are likely to undergo a pelvic ultrasound or MRI scan, to confirm the diagnosis.
There are two types of MRKH: Type 1 is the most common as identified by the characteristics above. Of those with Type 2 MRKH, 40% will have differences in the development of their kidneys (e.g. 15% have one kidney), 10% may have bone changes and another 10% may experience hearing difficulties.
Find out more about MRKH with information for patients, relatives and carers from the Imperial NHS Trust.
Mental Health and Wellbeing
Often a diagnosis of MRKH can affect your emotional wellbeing. Whilst this diagnosis can affect people in different ways and at different times, typically feelings of loss, grief and anger are reported. MRKH can sometimes be experienced as a trauma and can impact personal and sexual identity. You are not alone.
Knowing when and how to ask for help is important. It is OK to not be OK. Whether you choose to speak to friends, family, the MRKH community or a professional, or all of the above, is up to you but know that you are not alone. We are here to help and have also collated some Mental Health and Wellbeing resources for more information and tips to support your mental health regardless of where you are in your MRKH journey.
Making your own choices
Whether you choose to follow a path to lengthen your vagina or not is entirely up to you and there is absolutely no requirement to proceed with any treatment at all. This is completely your choice.
There are two main methods of treatment you can discuss with your doctor to find out more information about your case and discuss the options available:
- Dilation is the most common and least invasive route, and is successful in at least 95% of cases. Find out more about dilation here.
- Some clinicians offer surgery to create a vaginal passage which can often usually mean there is some form of dilation afterwards to keep the vagina open.
Some women use their partners to assist them in the creation of a vagina naturally through intercourse, but it is best to visit a specialist to check the safety of this route.
In all cases, the options available will likely vary depending on where you live. Most importantly, when and if to proceed with treatment is completely up to you, we are all different after all.
What does the future hold?
Being diagnosed, often as a teenager, with MRKH can make you think about what the future looks like much sooner than you expect. It can be terrifying to be confronted with this reality and not really understand what it means, what might happen and how it will affect you. We have compiled some resources to provide some more information on the options available whether you decide to have children or not.
The future is what we make it. Happiness comes in so many forms. Family comes in many forms. Not everyone sees children in their future, or indeed gets to that stage in their journey and there is nothing wrong with that.
Having MRKH can raise a lot of questions related to if you can still have children at all. The answer is yes you can.
In some cases, women with MRKH can still have their own biological child through In-Vitro Fertilisation (IVF), where your eggs can be removed and fertilised by your partner’s sperm and then placed in a surrogate’s uterus. This is known as IVF Surrogacy.
Other alternatives available are adoption and fostering. There are many agencies in the UK and globally that assist intended parents with and provide detailed information to start you on your journey.
There is also a lot of international research efforts into womb transplants. However, these are not a standard procedure offered nationwide / worldwide and trials are still ongoing.
We provide some useful links across our website where you can find out more about anything mentioned above and we will continue to add more information as it becomes available to cater to all, whatever age and stage of your journey.
Follow Us on Social Media